Why analyze patient data for personalized care in 2026
Discover why analyzing patient data is essential for personalized functional medicine and dietetics. Learn frameworks, overcome challenges, and leverage AI for better clinical outcomes.

Many functional medicine practitioners and dietitians hesitate to dive deep into patient data analysis, viewing it as time-consuming or overly complex. Yet this analytical approach is what separates truly personalized care from generic protocols. By systematically examining lab results, timelines, and lifestyle factors, you unlock the ability to detect imbalances early, identify root causes, and create treatment plans that actually work for each individual. This article reveals why patient data analysis is essential for delivering superior outcomes in functional medicine and dietetics, and how to implement it effectively without drowning in information overload.
Table of Contents
- Key takeaways
- The role of patient data analysis in functional medicine and dietetics
- Methodologies and frameworks for effective patient data analysis
- Navigating evidence, critiques, and the power of precision analytics
- Applying patient data analysis for personalized clinical decision-making
- Enhance clinical care with Meelio's AI-powered patient data analysis
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Early detection | Systematic analysis of labs, timelines, and lifestyle factors allows detection of imbalances before symptoms appear, enabling proactive interventions. |
| Root cause mapping | Synthesizing functional labs, genetics, and lifestyle data reveals root causes that standard tests miss, guiding personalized therapies. |
| Registries inform outcomes | Registries tracking nutrition outcomes strengthen clinical reasoning and policy development. |
| Balanced data use | Avoid overtesting by prioritizing markers linked to treatment decisions and expanding only as patterns emerge. |
The role of patient data analysis in functional medicine and dietetics
Analyzing patient data forms the foundation of effective functional medicine and nutrition practice. Functional lab tests detect subtle physiological imbalances before clinical symptoms emerge, giving you the opportunity to intervene at preclinical stages. This proactive approach transforms how you deliver care, moving from reactive symptom management to true prevention.
Patient data supports precise, individualized treatment plans that evolve with each person's progress. Standard protocols rarely account for the biochemical uniqueness each patient brings. By analyzing comprehensive data sets including functional labs, genetic markers, and lifestyle factors, you craft interventions tailored to specific imbalances rather than applying one-size-fits-all approaches.
For registered dietitians, patient data analysis via registries like the Academy of Nutrition and Dietetics Health Informatics Infrastructure tracks medical nutrition therapy outcomes using the Nutrition Care Process. This systematic approach provides evidence for decision-making and policy development. You gain insights into which nutrition interventions produce the best results across different patient populations, strengthening your clinical reasoning.
Data analysis promotes personalized nutrition interventions that dramatically improve patient adherence and outcomes. When patients see their biomarkers improving in response to specific dietary changes, motivation increases. You can demonstrate cause and effect relationships between nutrition choices and health metrics, making abstract concepts tangible.
Pro Tip: Start with a focused data set rather than ordering every available test. Prioritize markers that directly inform treatment decisions for the patient's primary concerns, then expand analysis as patterns emerge requiring deeper investigation.
Careful synthesis of multi-source data proves critical for effective clinical application. Raw numbers mean little without context from patient history, symptoms, and lifestyle factors. Patient-centered care in functional medicine requires integrating quantitative data with qualitative information to form a complete clinical picture. Your analytical skills transform disparate data points into actionable treatment strategies.
The real power emerges when you connect seemingly unrelated findings. A patient's elevated inflammatory markers might link to gut dysbiosis revealed in microbiome testing, which connects to food sensitivities identified through elimination protocols. Functional nutrition checklists help ensure you capture all relevant data points systematically, preventing important details from slipping through the cracks during busy clinical days.
Methodologies and frameworks for effective patient data analysis
The Functional Medicine Matrix provides a systems biology framework that maps relationships between body systems and environmental factors. This visual tool helps you organize complex patient data by categorizing information into defense and repair, energy, biotransformation, communication, transport, and structural integrity. Each category connects to antecedents, triggers, and mediators that influence patient health.
Timeline mapping traces the sequence of events leading to current health issues. You document when symptoms first appeared, what preceded them, and which factors perpetuate the condition. This chronological approach reveals cause-effect relationships that static lab snapshots miss. A patient's autoimmune condition might trace back to antibiotic use years earlier, followed by chronic stress, then specific dietary exposures.

Systems biology healthcare outcomes improve when you apply these frameworks systematically. The methodology transforms overwhelming amounts of patient information into organized, actionable intelligence. Thinking functionally beyond protocols requires mastering these analytical frameworks to handle complex cases effectively.
Targeted specialized labs identify root causes that standard testing overlooks:
- GI-MAP stool testing reveals bacterial overgrowth, parasites, and inflammatory markers affecting gut health
- DUTCH hormone testing maps cortisol patterns and sex hormone metabolism throughout the day
- Organic Acids Test evaluates mitochondrial function, neurotransmitter metabolism, and nutritional deficiencies
- Micronutrient panels assess intracellular vitamin and mineral status beyond serum levels
| Framework | Primary Use | Key Advantage |
|---|---|---|
| Functional Medicine Matrix | Systems mapping | Visualizes interconnections between body systems |
| Timeline Analysis | Causation tracking | Identifies triggers and perpetuating factors |
| Specialized Labs | Root cause detection | Reveals subclinical imbalances |
| Nutrition Care Process | Outcome monitoring | Standardizes dietetic practice and evidence collection |
Balancing comprehensive analysis with clinical judgment prevents excessive testing and interpretation errors. Not every patient needs every test. Efficient patient management workflow prioritizes testing based on clinical presentation and treatment response. You order additional labs when initial interventions produce unexpected results or when symptoms suggest specific underlying mechanisms.
Pro Tip: Create a decision tree for test ordering based on chief complaints and initial findings. This systematic approach ensures thorough investigation while avoiding the shotgun testing approach that overwhelms both you and your patients financially and cognitively.
These methodologies enable you to formulate comprehensive, personalized treatment protocols addressing multiple body systems simultaneously. A patient with chronic fatigue might need gut repair, adrenal support, mitochondrial optimization, and blood sugar stabilization. Your data analysis reveals which systems require priority attention and how interventions should sequence for maximum effectiveness.
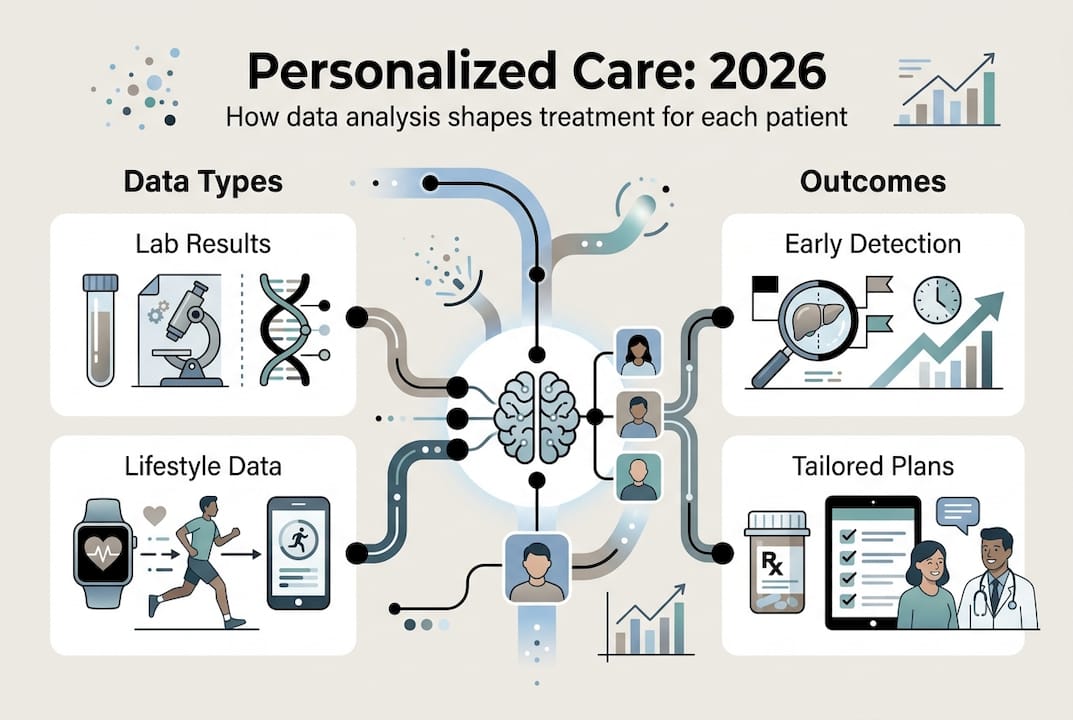
Navigating evidence, critiques, and the power of precision analytics
Functional medicine faces legitimate scrutiny regarding its evidence base. Critics question validation of certain tests and cite lack of randomized controlled trials for individualized approaches. Concerns center on unvalidated tests like adrenal fatigue panels, potential over-testing driven by profit motives, and reliance on testimonials rather than rigorous research. These critiques deserve serious consideration as you develop your analytical approach.
Proponents counter that functional medicine's individualized root-cause focus produces superior outcomes for chronic diseases where conventional medicine struggles. The personalization inherent in functional approaches makes traditional RCT methodology challenging. How do you randomize treatments when each patient receives a unique protocol based on their specific imbalances? This tension between evidence standards and clinical reality creates ongoing debate.
"Contrasting viewpoints exist: Proponents claim superior chronic outcomes via root-cause focus; critics label it pseudoscience with unvalidated tests, over-testing, profit-driven practices, and lacking RCTs due to personalization challenges."
Emerging AI and subphenotyping from electronic health record data offer solutions to evidence concerns. Using EHR data for subphenotyping improves predictions in complex diseases like Crohn's disease and non-small cell lung cancer. These precision analytics identify patient subgroups that respond differently to treatments, validating the personalized medicine approach with data-driven methodology.
Systems thinking proves critical for managing complex, contradictory clinical data that protocols cannot address:
- Messy lab results with some markers elevated and others normal require contextual interpretation
- Contradictory symptoms suggesting multiple competing mechanisms need systematic analysis
- Compensatory patterns where the body adapts to dysfunction, masking underlying problems
- Individual variations in metabolism affecting standard reference range applicability
AI in functional medicine enhances your ability to recognize these patterns across large datasets. Machine learning algorithms identify subtle correlations between biomarkers, symptoms, and outcomes that human analysis might miss. Clinical intelligence AI processes thousands of patient records to suggest which combinations of findings predict specific conditions or treatment responses.
| Approach | Evidence Strength | Practical Application | Limitation |
|---|---|---|---|
| Conventional Testing | High (RCT-based) | Disease diagnosis | Misses subclinical dysfunction |
| Functional Testing | Mixed (mechanistic + observational) | Root cause identification | Some tests lack validation |
| AI Subphenotyping | Emerging (large datasets) | Precision predictions | Requires extensive data |
| Hybrid Model | Strongest (combines approaches) | Comprehensive care | Complexity in integration |
Balanced approaches integrating conventional and functional models address both evidence and practical concerns. You use standard labs for baseline assessment and disease monitoring while adding functional tests when clinical presentation suggests specific mechanisms. This hybrid strategy maintains scientific rigor while expanding diagnostic capabilities.
The key lies in transparent communication with patients about test validity and evidence levels. Explain which tests have robust validation and which provide mechanistic insights requiring clinical correlation. This honesty builds trust while acknowledging the evolving nature of functional medicine evidence. Your role includes staying current with emerging research that either validates or questions specific testing methodologies.
Applying patient data analysis for personalized clinical decision-making
Empirical benchmarks guide how you allocate time and intervention intensity. Higher malnutrition risk correlates with increased registered dietitian care time, with high-risk pediatric patients requiring 31% more attention than lower-risk cases. Better documentation predicts diagnosis improvement, emphasizing the importance of thorough data recording. These findings help you justify appropriate time investments for complex cases.
Integrate patient registries and outcome data to monitor nutrition care process effectiveness:
- Document baseline biomarkers, symptoms, and functional status at intake
- Track intervention details including dietary protocols, supplements, and lifestyle modifications
- Measure outcomes at consistent intervals using standardized assessments
- Compare individual results against registry benchmarks to identify outliers
- Adjust protocols based on response patterns across your patient population
Balance comprehensive data gathering with avoiding over-testing through clinical judgment and patient-centered focus. Crafting effective care plans requires selecting tests that directly inform treatment decisions rather than satisfying curiosity. Ask yourself whether each test result would change your treatment approach. If the answer is no, reconsider ordering it.
Incorporate lifestyle and stress management data alongside lab results for holistic personalization. Cortisol patterns mean little without understanding work schedules, sleep quality, and stress perception. A patient's elevated inflammatory markers might stem more from chronic sleep deprivation than dietary factors. Your analysis must weigh biological data against behavioral and environmental contexts.
Pro Tip: Create a data integration template that includes sections for labs, symptoms, lifestyle factors, and patient goals. This structured approach ensures you consider all relevant information when developing treatment plans rather than fixating on lab abnormalities alone.
Apply automated workflows and AI care plans to streamline data integration and clinical decision-making. Manual data synthesis consumes hours that could go toward patient interaction. Workflow automation in functional medicine handles routine analysis tasks, flagging significant findings and suggesting evidence-based interventions. You retain final decision authority while benefiting from computational support.
Meal planning improves adherence when personalized based on patient data. Your analysis reveals which foods trigger inflammation, which nutrients need emphasis, and which dietary patterns suit the patient's lifestyle. Data-driven meal plans feel less restrictive because patients understand the specific reasons behind each recommendation. They see how their unique biochemistry requires particular nutritional strategies.
Successful patient data analysis requires continuous learning and adaptation. New testing methodologies emerge regularly, research updates understanding of biomarker significance, and patient responses teach you which patterns predict outcomes. Build feedback loops into your practice where treatment results inform future analytical approaches. Track which initial findings most reliably predict treatment success, allowing you to refine your assessment priorities over time.
Enhance clinical care with Meelio's AI-powered patient data analysis
You've learned how patient data analysis transforms functional medicine and nutrition practice, but implementing these strategies manually consumes precious clinical hours. Meelio provides AI-driven tools specifically designed for integrative and functional health practitioners who need to leverage patient data without drowning in administrative work.
Our platform automates longitudinal lab analysis, generates protocol-specific care plans for frameworks like Bredesen and Wahls, and creates personalized nutrition recommendations based on your patient's unique data profile. Meelio's AI assistant integrates with your existing EHR systems like Practice Better and Cerbo, transforming raw patient data into actionable clinical intelligence. Practitioners using our platform save over four hours daily while delivering more precise, individualized care. Explore AI care plans for treatment planning to see how clinical intelligence automation enhances your analytical capabilities and patient outcomes.
Frequently asked questions
What types of patient data are most valuable to analyze in functional medicine?
The most valuable data includes functional lab results like GI-MAP for gut health, DUTCH for hormone patterns, and Organic Acids Test for metabolic function. Clinical history timelines revealing symptom onset and progression provide essential context. Lifestyle factors including diet quality, sleep patterns, stress levels, and exercise habits complete the picture. Combining quantitative biomarkers with qualitative patient experiences creates comprehensive profiles that inform truly personalized treatment strategies.
How can registered dietitians use patient data to improve nutrition care outcomes?
Dietitians utilize registries following the Nutrition Care Process to systematically track patient outcomes and refine medical nutrition therapy interventions. Best nutrition software platforms help organize client data for evidence-based adjustments. Data-driven modifications to meal plans and supplement protocols improve both adherence and clinical effectiveness. Tracking biomarker changes in response to specific dietary interventions demonstrates value to patients and builds your evidence base for future cases.
What are common challenges when analyzing patient data in functional medicine?
Practitioners face data overload from multiple testing modalities producing hundreds of individual markers. Contradictory lab results where some markers suggest one condition while others point elsewhere create interpretation difficulties. The temptation toward over-testing wastes resources and overwhelms patients. Integrating systems biology frameworks like the Functional Medicine Matrix helps organize complex information. Clinical judgment developed through experience guides which findings deserve focus versus which represent normal variation or compensatory adaptations.
How does AI improve patient data analysis in functional medicine?
AI enables integration of massive datasets across thousands of patients to identify patterns invisible to individual practitioners. Subphenotyping algorithms group patients by response characteristics, predicting which treatments will work for specific profiles. AI in functional medicine reduces the cognitive load of synthesizing multiple data sources while enhancing diagnostic precision. Predictive analytics forecast disease progression and treatment outcomes based on baseline data. These capabilities allow you to deliver more precise care in less time, addressing both effectiveness and efficiency challenges in complex case management.





