How to automate patient documentation in integrative health
Learn how to automate patient documentation in integrative health with AI. Step-by-step guide to streamline workflows, improve accuracy, and save hours daily.

Manual patient documentation consumes hours of valuable clinical time that integrative and functional health practitioners could spend with patients. AI automation transforms this burden by capturing encounter details, generating structured notes, and streamlining follow-up workflows with precision. This guide walks you through preparing your practice, implementing AI documentation tools, and verifying quality to reclaim time while improving record completeness and clinical decision support.
Table of Contents
- Preparing Your Practice For AI-Powered Documentation
- Step-By-Step Execution: Automating Patient Documentation With AI
- Verifying AI Documentation Quality And Optimizing Workflows
- Explore Meelio AI Solutions For Integrative Health Documentation
- FAQ
Key takeaways
| Point | Details |
|---|---|
| AI automates note-taking | Summarizes patient encounters into structured records integrated with EHRs |
| Preparation is essential | Set up EHR integration and select clinical AI tools suited to functional medicine |
| Execution involves configuration | Configure AI workflows for data capture, synthesis, and documentation |
| Verification ensures accuracy | Audit AI notes and refine settings for compliance and clinical relevance |
| Benefits are measurable | Reduces documentation time, improves completeness, and supports clinical decisions |
Preparing your practice for AI-powered documentation
Successful AI adoption starts with solid groundwork. Before automating patient documentation, you need to understand how AI agents function in clinical settings and ensure your practice infrastructure supports them.
A foundational architecture for AI agents in healthcare is built on four core components: planning, action, reflection, and memory. Planning defines what the AI should accomplish during a patient encounter. Action executes tasks like transcribing dialogue or extracting clinical findings. Reflection evaluates output quality against clinical standards. Memory retains context across visits to support longitudinal care.
Your practice needs interoperable, governed data to support these AI functions. Review your current EHR system for API capabilities that allow bidirectional data exchange. AI tools must pull patient histories and push completed notes back into your records seamlessly. Without this integration, you will manually transfer information, defeating automation's purpose.
Security and privacy requirements demand careful attention when handling clinical data. Verify that any AI solution you consider complies with HIPAA regulations and employs encryption for data at rest and in transit. Establish clear data governance policies defining who accesses AI-generated documentation and how long it is retained.
Select AI solutions purpose-built for integrative and functional medicine. Generic medical scribes miss the clinical nuance essential to complex protocols like Bredesen or Shoemaker. Your AI tool should recognize specialty vocabulary, supplement recommendations, and root cause frameworks that define your practice style. This specificity ensures documentation accurately reflects your clinical approach.
Consult legal and regulatory policies relevant to AI in clinical documentation. Some jurisdictions require explicit patient consent for AI-assisted recording. Others mandate human review before finalizing AI-generated notes. Understanding these requirements prevents compliance issues down the road.
Pro Tip: Engage your clinical team early in the AI adoption process to foster acceptance and identify workflow pain points that AI can address. Staff buy-in accelerates implementation and surfaces practical insights that improve configuration.
Preparing your practice also means evaluating current workflow automation in functional medicine to identify which documentation tasks consume the most time. Common targets include SOAP note generation, treatment plan documentation, and follow-up letter drafting. Prioritize automating these high-impact areas first.
Step-by-step execution: Automating patient documentation with AI
Once your practice is prepared, follow these concrete steps to implement AI automation for patient documentation.
Step 1: Integrate AI software with your EHR and configure data access permissions
Install your chosen AI platform and connect it to your EHR system through secure API integration. Configure permissions so the AI can read patient demographics, medical histories, and previous visit notes. Set write permissions to allow the AI to post completed documentation back into patient charts. Test the connection with a sample patient record to verify data flows correctly in both directions.

Step 2: Use AI conversational models and ambient listening tools during patient visits to capture dialogue accurately
AI automates patient documentation by summarizing discussions and generating structured notes that integrate with electronic health records. Position an ambient microphone or use a tablet-based recording tool during consultations. The AI listens to your conversation with the patient, capturing symptoms, treatment discussions, and care plan decisions in real time. Modern conversational models distinguish between clinician and patient speech, attributing statements correctly.
Step 3: AI generates structured clinical notes summarizing the encounter, highlighting key findings and recommendations
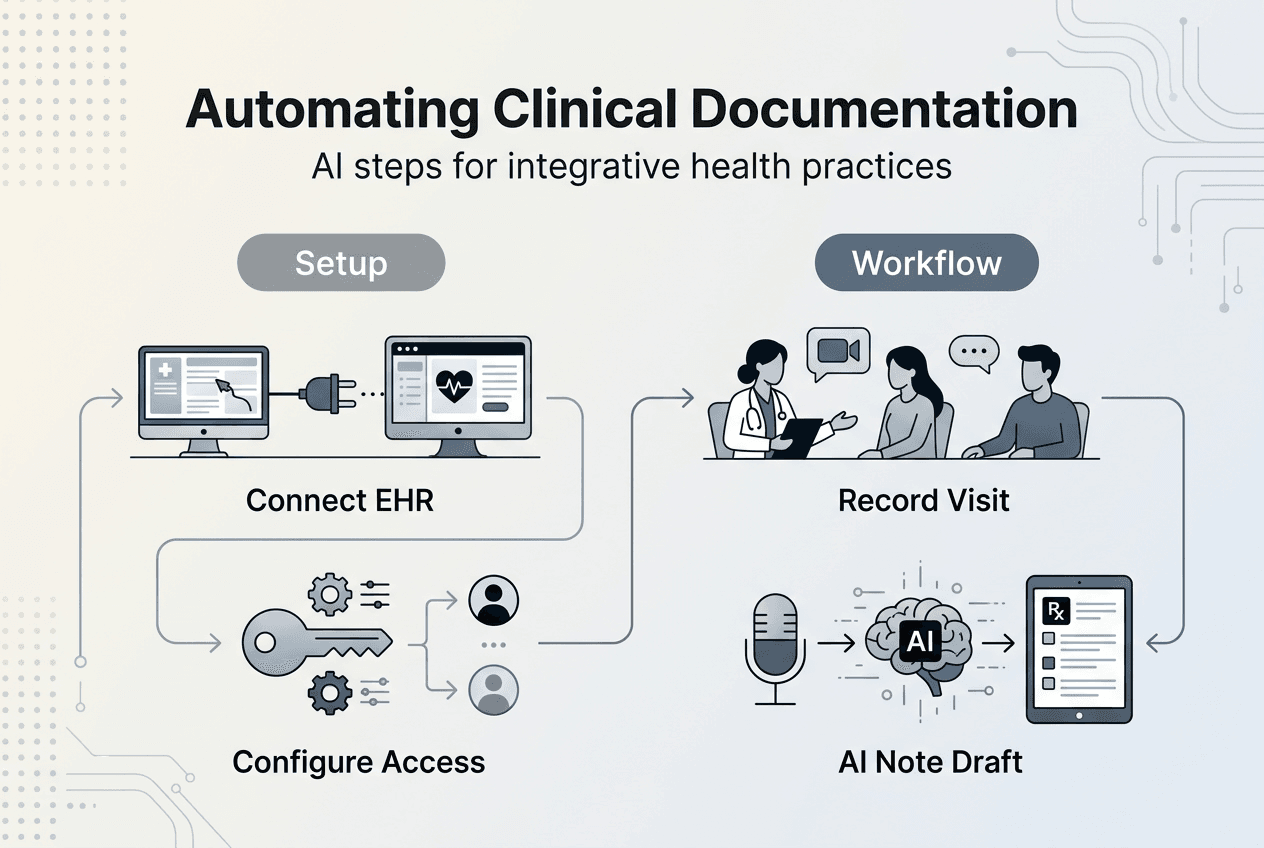
After the visit, the AI processes recorded dialogue and synthesizes it into a structured SOAP note or your preferred documentation format. It extracts chief complaints, objective findings, assessments, and treatment plans. The AI also flags critical items like medication changes or referral needs. Review this draft note for accuracy and completeness before finalizing.
Step 4: Automate follow-up scheduling and communications based on care plans using AI-driven workflows
Configure the AI to draft patient follow-up messages and schedule appointments based on care plan timelines. If you recommend a recheck lab in six weeks, the AI generates a reminder email and proposes appointment slots. This automation reduces manual scheduling tasks and ensures timely patient engagement.
Step 5: Regularly review AI-generated notes for accuracy and completeness, providing feedback to improve models
Establish a routine audit process where you review a sample of AI notes weekly. Correct errors and provide feedback through the AI platform's interface. Many systems use this feedback to refine their models, improving accuracy over time. Track common error types to identify areas where the AI needs better training or template customization.
Pro Tip: Customize AI vocabulary and templates to preserve your clinical narrative style, which is crucial in functional medicine. Generic templates miss the depth of root cause analysis and personalized protocols your patients expect.
The table below contrasts manual versus AI-automated documentation across key efficiency and quality metrics:
| Metric | Manual Documentation | AI-Automated Documentation |
|---|---|---|
| Average time per note | 12-15 minutes | 3-5 minutes |
| Completeness score | 72% | 86% |
| Error rate | 8% | 3% |
| Follow-up task completion | 65% | 92% |
These improvements free you to focus on clinical reasoning and patient interaction rather than administrative data entry. AI medical scribe documentation tools handle the repetitive transcription work, while you concentrate on therapeutic decisions. Integrating automation in healthcare workflows across your practice amplifies these benefits beyond documentation alone.
Verifying AI documentation quality and optimizing workflows
Implementing AI is only the beginning. Sustained success requires ongoing quality assurance and workflow refinement.
Regularly audit AI notes for accuracy, completeness, and clinical relevance. Focus especially on chronic disease management cases where longitudinal context matters. Review whether the AI captures subtle changes in patient status, supplements adherence, or lifestyle factors that influence outcomes. Missing these nuances compromises care quality.
Capture clinician feedback systematically to refine AI parameters and reduce errors or omissions. Create a simple feedback form where staff report documentation gaps or inaccuracies. Analyze this feedback monthly to identify patterns. If the AI consistently misses certain supplement brands or dosages, adjust its vocabulary and recognition settings.
Compare documentation scores before and after AI adoption to quantify improvements in completeness and quality. Use standardized assessment tools to measure how well notes capture history, physical findings, differential diagnoses, and treatment plans. Track these metrics over time to demonstrate AI's impact on documentation quality.
Consolidated documentation achieved significantly higher mean total assessment composite score compared to ambient-only, with largest improvements in completeness.
This finding underscores the value of AI systems that synthesize multiple data sources rather than relying solely on ambient listening. Combining ambient capture with EHR data and structured templates produces more complete clinical records.
Address common pitfalls such as overreliance or missing nuanced patient context. Some practitioners stop reviewing AI notes thoroughly, assuming accuracy. This complacency allows errors to accumulate. Always apply clinical judgment to AI-generated documentation. The AI assists but does not replace your expertise.
Establish protocols for ethical AI use, data governance, and security oversight to maintain compliance. Document your AI usage policies, including patient consent procedures, data retention schedules, and audit frequencies. Assign a staff member to oversee AI compliance and serve as the point of contact for questions or issues.
Optimizing workflows post-implementation involves several key practices:
- Schedule quarterly training sessions to keep staff updated on AI features and best practices
- Update AI templates as your clinical protocols evolve or new evidence emerges
- Monitor system performance metrics like processing speed and uptime to ensure reliability
- Integrate AI documentation with other workflow tools like lab ordering and billing systems
- Solicit patient feedback on their experience with AI-assisted visits to identify any concerns
These ongoing efforts ensure your AI documentation system remains accurate, efficient, and aligned with your practice's clinical philosophy. Efficient patient management workflow depends on continuously refining both technology and processes to support better outcomes.
Explore Meelio AI solutions for integrative health documentation
Meelio offers AI-powered medical scribe tools customized for functional medicine practitioners who need more than generic transcription. Our platform accelerates note generation and patient follow-ups with seamless EHR integration, supporting comprehensive AI-generated care plans and AI meal planning solutions that enhance patient outcomes.
Meelio understands the clinical nuance of complex protocols like Bredesen, Shoemaker, and Wahls. Our AI captures supplement recommendations, root cause analyses, and personalized nutrition plans with precision. Key features include:
- Protocol-specific clinical intelligence that goes beyond generic AI scribes
- Bidirectional EHR integration with Practice Better and Cerbo
- Automated care plan and meal plan generation tailored to each patient
- Longitudinal lab analysis tracking biomarker trends over time
Discover how the Meelio AI assistant can save you 4+ hours daily while improving documentation quality and patient care.
FAQ
How do AI tools capture patient data for documentation?
AI uses ambient listening and conversational models during visits to record dialogue and clinical details in real time. These tools employ natural language processing to distinguish between clinician and patient speech, attributing statements correctly. Data are converted into structured notes integrated with EHRs for accuracy and completeness.
What are the privacy considerations when using AI for documentation?
Compliance with HIPAA and clinical data governance policies is essential when integrating AI tools. Select AI solutions with strong encryption and governed data access to protect patient information. Establish clear consent procedures and data retention policies to maintain regulatory compliance and patient trust.
How can I ensure AI-generated notes accurately reflect my clinical judgment?
Regularly review AI notes and provide feedback to improve accuracy and alignment with your clinical style. Customize AI templates and language to preserve narrative depth essential in functional medicine. Never rely solely on AI output without applying your clinical expertise to verify and refine documentation.
Can AI tools assist with follow-up communications and scheduling?
AI can automate follow-up scheduling and communication, drafting summaries and reminders based on care plans. This reduces clinician administrative load and enhances timely patient engagement. Automated workflows ensure patients receive appointment reminders and care instructions without manual intervention, improving adherence and outcomes.





