How to Manage Bredesen ReCODE Documentation with AI: A 2026 Guide
7.2M Americans have Alzheimer's. Learn how AI streamlines Bredesen ReCODE documentation across 150 variables, 6 subtypes, and longitudinal cognitive tracking.
How to Manage Bredesen ReCODE Protocol Documentation with AI: A 2026 Guide
The scale of cognitive decline is staggering. An estimated 7.2 million Americans age 65 and older will be living with Alzheimer's in 2025, a figure projected to nearly double by 2060 (Alzheimer's Association, 2025). This crisis carries a total economic burden of $781 billion in the U.S. alone (USC Schaeffer Center, 2025). As functional medicine clinicians, we are uniquely positioned to address this with comprehensive, root-cause approaches like the Bredesen ReCODE protocol.
The protocol's strength, however, is also its primary documentation challenge. It requires evaluating over 150 variables to identify a patient's specific cognitive decline subtype. This creates a massive data management and charting burden. This guide provides a step-by-step process for using AI to streamline ReCODE documentation, saving you time while improving patient care. With studies showing that 74% of ReCODE participants showed cognition stabilized or improved (Biomedicines/MDPI, 2021), optimizing our workflow is essential to delivering these outcomes at scale.
Key Takeaways
- The Bredesen ReCODE protocol evaluates 150 variables across 6 cognitive decline subtypes (Apollo Health, 2024).
- Clinical trials show that 74% of protocol participants had cognition that stabilized or improved (Biomedicines, 2021).
- AI documentation tools can reduce clinician burnout from 51.9% to 38.8% (PMC/JAMA, 2025).
- Nearly 24% of the global population carries at least one APOE4 allele, a key genetic risk factor for Alzheimer's (Journal of Alzheimer's Disease, 2021).
Why Does the Bredesen Protocol Generate So Much Documentation?
The Bredesen protocol generates immense documentation because it evaluates over 150 different variables across biochemistry, genetics, and imaging (Apollo Health, 2024). This complexity is necessary to identify a patient's root causes and dominant subtype of cognitive decline, but it places a significant administrative load on clinicians. The protocol is not a single intervention; it's a personalized program tailored to the individual's unique physiology.
The initial workup, or "cognoscopy," is exhaustive. It includes a deep explore blood biomarkers for inflammation and metabolic health, genetic testing for risks like the APOE4 allele, and advanced imaging such as volumetric MRIs. We also conduct detailed cognitive assessments like the Montreal Cognitive Assessment (MoCA). Each of these data points must be captured, interpreted, and tracked over time.
This process is repeated and adjusted based on which of the six subtypes presents: Inflammatory (Hot), Atrophic (Cold), Glycotoxic (Sweet), Toxic (Vile), Vascular (Pale), or Traumatic (Dazed). A standard SOAP note simply cannot contain this level of detail. Given that physicians already spend nearly 13 hours per week on indirect patient care (AMA, 2024), how can we manage this additional burden without burning out?
Step 1: Build a Cognoscopy Assessment Template
A structured cognoscopy template is your foundation, and AI can build it from your existing notes or a simple prompt. The Montreal Cognitive Assessment (MoCA) is a critical component, demonstrating 90.2% sensitivity in detecting cognitive impairment compared to just 78.4% for the MMSE (PubMed, 2025). An effective AI-powered template should organize data collection around this and other key ReCODE pillars.
Your template should include dedicated sections for exposure history (mold, toxins), genetic risk factors (APOE4 status), comprehensive metabolic panels, and cognitive testing scores. This initial structure ensures you capture all 150 potential variables systematically. It moves beyond a simple history and physical, creating a dynamic record of a patient’s neurological health baseline.
Crucially, categorize biomarkers by their relevance to the six subtypes. For example, group hs-CRP and homocysteine under "Inflammatory," key hormone levels under "Atrophic," HOMA-IR and fasting insulin under "Glycotoxic," and mycotoxin or heavy metal panels under "Toxic." Generic EHR templates fail because they lack the specificity to map these functional labs directly to the Bredesen subtypes. An AI assistant trained on functional medicine protocols can build this for you.
Step 2: Configure Subtype-Specific Lab Review Templates
AI can create lab review notes that interpret results through the specific lens of each ReCODE subtype. This is essential because nearly 23.9% of the global population carries at least one APOE4 allele, a variant that dramatically changes how we interpret other biomarkers like lipids and inflammatory markers (Journal of Alzheimer's Disease, 2021). Your documentation must reflect this genetic context.
Each of the six subtypes is driven by different biological mechanisms, requiring distinct biomarker panels and interpretations. A patient with Type 1 (Inflammatory) cognitive decline needs a note focused on trends in hs-CRP and homocysteine. In contrast, a patient with Type 1.5 (Glycotoxic) requires an interpretation centered on insulin resistance markers. A generic lab summary is clinically insufficient.
Use AI to generate templates that automatically pull in relevant biomarkers for each subtype. This includes tracking C-reactive protein, homocysteine, fasting insulin, vitamin D, B12, testosterone, estradiol, and specific toxins. The AI can be trained to use functional ranges, not just standard lab ranges, providing a more precise clinical picture. This approach creates phase-aware documentation that adapts as the patient's primary subtype drivers shift during treatment.
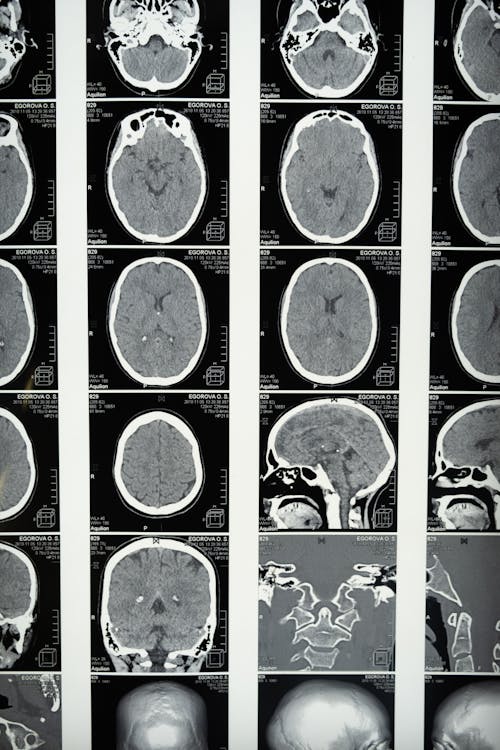
Step 3: Automate ReCODE Care Plans by Subtype
You can use AI to draft personalized ReCODE care plans based on a patient's determined subtype, saving hours of manual work. With studies showing 74% of participants demonstrating stabilized or improved cognition (Biomedicines/MDPI, 2021), efficiently creating and deploying these targeted plans is key to achieving similar results in your practice. The goal is to translate complex cognoscopy data into an actionable, subtype-specific protocol.
Map each of the six subtypes to a corresponding care plan template within your AI system. This allows for rapid generation of a baseline protocol that you can then refine. For instance, a finding of Type 1 (Inflammatory) would trigger an AI-generated plan focused on a comprehensive anti-inflammatory protocol, gut health restoration using the 4R program, and specific dietary changes.
For a patient with Type 1.5 (Glycotoxic) or "Sweet" cognitive decline, the AI would instead generate a plan emphasizing insulin sensitization strategies, exercise recommendations, and the Ketoflex 12/3 diet. This is where phase-aware documentation becomes powerful. The AI understands the patient's subtype and current treatment phase, ensuring the generated plan is always clinically relevant. This frees you to focus on nuanced adjustments and patient coaching rather than repetitive typing.
Step 4: Generate Ketoflex 12/3 Meal Plans from Patient Data
AI can generate patient-specific Ketoflex 12/3 meal plans, a core dietary intervention in the ReCODE protocol. With physician AI usage rising from 38% to 66% between 2023 and 2024 (AMA, 2025), tools that automate complex but routine tasks like meal planning are becoming standard. This allows for greater personalization and adherence.
The Ketoflex 12/3 diet is a plant-rich, mildly ketogenic approach. It incorporates a fasting window of at least 12 hours overnight, with the final meal consumed at least 3 hours before bed. This strategy is designed to improve insulin sensitivity, reduce inflammation, and promote autophagy, which are critical for patients with Glycotoxic or Inflammatory subtypes. But how do you make this practical for each patient?
Instead of providing generic food lists, an AI assistant can use the patient's chart data, including food sensitivities, allergies, and preferences, to create a customized weekly meal plan. You can simply instruct the AI: "Generate a 7-day Ketoflex 12/3 meal plan for this patient, avoiding gluten and dairy." The system produces a detailed plan with recipes that you can quickly review and share, dramatically improving the patient experience and likelihood of success.

Step 5: Track Cognitive Outcomes Across Protocol Phases
Use AI to facilitate the longitudinal tracking of cognitive scores and biomarkers, a critical step for demonstrating progress and adjusting protocols. A landmark 2025 randomized controlled trial showed statistically significant improvements in cognitive index, memory, and executive function for patients on the protocol (Apollo Health/JAD, 2025). Meticulous tracking is how we replicate these results in a clinical setting.
Your AI documentation system should be configured to easily compare data over time. This includes trend analysis of MoCA scores, key blood markers like hs-CRP or fasting insulin, and even changes in volumetric MRI reports. The AI can pull data from previous encounters into the current note, allowing you to quickly see a patient's trajectory. For example, your follow-up note can automatically include the MoCA score from three and six months prior for immediate comparison.
This longitudinal data is the foundation for clinical decision-making. If a patient with the Atrophic subtype isn't showing improvement in cognitive scores after three months of hormone optimization, the data makes it clear that a protocol adjustment is needed. The AI doesn't make the decision, but it organizes the exact information you need to apply your clinical judgment effectively.
Common Mistakes in ReCODE Documentation
Even with advanced tools, several common documentation pitfalls can undermine the ReCODE protocol's effectiveness. Avoiding these mistakes ensures your records accurately reflect the personalized, subtype-driven nature of the treatment.
First, many clinicians fail to tag notes and care plans with the patient's specific subtype. This makes it difficult to track interventions and outcomes for Type 1 versus Type 3 patients over time. Second, they rely on standard lab reference ranges instead of the optimal functional ranges required by the protocol. This can lead to missed opportunities for intervention.
Another frequent error is not documenting adherence to the Ketoflex 12/3 diet or other lifestyle modifications. This information is crucial context for interpreting changes in biomarkers and cognitive scores. Finally, the biggest mistake is treating the protocol as a monolithic, one-size-fits-all checklist. Effective documentation must reflect the dynamic, personalized adjustments made based on a patient's unique response.

Frequently Asked Questions
How many variables does the Bredesen ReCODE protocol track?
The Bredesen ReCODE protocol is highly comprehensive, evaluating over 150 different variables for each patient (Apollo Health, 2024). This includes a wide range of blood biomarkers, genetic data like APOE status, cognitive test scores, and findings from advanced imaging like volumetric MRIs to build a complete picture of neurological health.
Can AI generate subtype-specific care plans without practitioner oversight?
No, AI should be used as a clinical assistant, not a replacement for your judgment. While it can draft a care plan based on a patient's subtype, the final protocol must be reviewed, customized, and approved by the clinician. The AI automates the routine parts of documentation, freeing you to focus on complex clinical reasoning.
What cognitive assessments should be tracked longitudinally?
The Montreal Cognitive Assessment (MoCA) is a primary tool for longitudinal tracking due to its high sensitivity. It demonstrates 90.2% sensitivity in detecting cognitive impairment, making it superior for monitoring subtle changes over time compared to other screeners (PubMed, 2025). This should be combined with tracking subjective patient-reported outcomes.
How long does a typical ReCODE protocol take to show results?
Results vary based on the patient's subtype, adherence, and baseline cognitive status. However, a key study demonstrated that 74% of 255 participants showed cognition that had either stabilized or improved (Biomedicines/MDPI, 2021). Most clinicians look for initial biomarker and cognitive shifts within the first 3-6 months.
Which EHRs support Bredesen protocol documentation?
Many modern, cloud-based EHRs like Cerbo and Practice Better can be adapted for ReCODE documentation. However, their built-in templates often lack the specificity needed. The most effective approach is to use an AI documentation layer that integrates with your EHR to manage the protocol's complexity.
Explore Cognitive Health Protocol Documentation with Meelio
Managing the data-intensive Bredesen ReCODE protocol requires more than a standard EHR. It demands a system built for the complexity of functional medicine. Meelio is an AI assistant designed specifically for clinicians like you, with capabilities for AI-driven medical scribing, subtype-aware care plans, and automated Ketoflex 12/3 meal planning.
By automating the administrative burden of ReCODE, you can dedicate more time to the clinical analysis and patient coaching that drive outcomes. See how a protocol-specific AI can enhance your cognitive health practice.





