Master the meal planning process for dietitians in 2026
Learn the complete meal planning process for dietitians, blending Nutrition Care Process with functional medicine to improve patient adherence and clinical outcomes.

Dietitians juggle complex patient needs, conflicting dietary preferences, and evolving clinical evidence while trying to create meal plans that patients actually follow. Without a structured yet flexible process, meal planning becomes reactive guesswork rather than strategic care. This guide walks you through a proven framework blending the Nutrition Care Process with functional medicine insights, showing you how to personalize plans efficiently, monitor outcomes effectively, and leverage technology to save hours weekly while improving patient adherence and clinical results.
Table of Contents
- Key takeaways
- Understanding the foundational Nutrition Care Process for meal planning
- Personalizing meal plans: blending traditional and functional medicine approaches
- Executing the meal planning process efficiently while maintaining flexibility
- Verifying results: monitoring, evaluation, and continuous improvement of meal plans
- Enhance your meal planning with Meelio AI assistant
- FAQ
Key Takeaways
| Point | Details |
|---|---|
| NCP framework | A four step process guides meal planning from assessment through evaluation to create accountable, measurable patient outcomes. |
| Personalization and flexibility | Tailor meal plans to patient preferences and real world constraints to improve adherence. |
| Functional medicine integration | Incorporate root cause analysis and lab insights to enhance plan relevance. |
| Ongoing monitoring | Track adherence outcomes and adjust plans using AI tools to save time. |
| AI planning automation | Leverage AI to automate planning tasks and flag patients needing attention. |
Understanding the foundational Nutrition Care Process for meal planning
The Nutrition Care Process provides a standardized framework that transforms meal planning from intuition-based practice into systematic, evidence-driven care. This model structures your clinical thinking through four interconnected steps that create accountability and measurability in patient outcomes.
Nutrition Assessment forms your foundation. You gather comprehensive data including medical history, current medications, lifestyle patterns, dietary intake analysis, and relevant biochemical markers. This isn't just chart review, it's detective work. You're identifying patterns between symptoms, eating behaviors, and health status that reveal intervention opportunities.
Nutrition Diagnosis translates assessment data into specific, actionable problems. Rather than vague observations, you document precise nutrition-related issues using standardized terminology. For example, "excessive carbohydrate intake related to limited cooking skills as evidenced by HbA1c of 8.2%" creates a clear target for intervention.
Nutrition Intervention is where meal planning happens. You design eating patterns tailored to diagnosed problems, patient preferences, cultural considerations, and practical constraints. This step includes education, goal setting, and creating the actual meal framework patients will follow. Your plans must balance clinical necessity with real-world feasibility.
Pro Tip: Document specific barriers during assessment, like work schedules or family meal dynamics, then reference these directly in your intervention notes. This creates continuity between what you learned and how you're addressing it, making plan adjustments more logical and defensible.
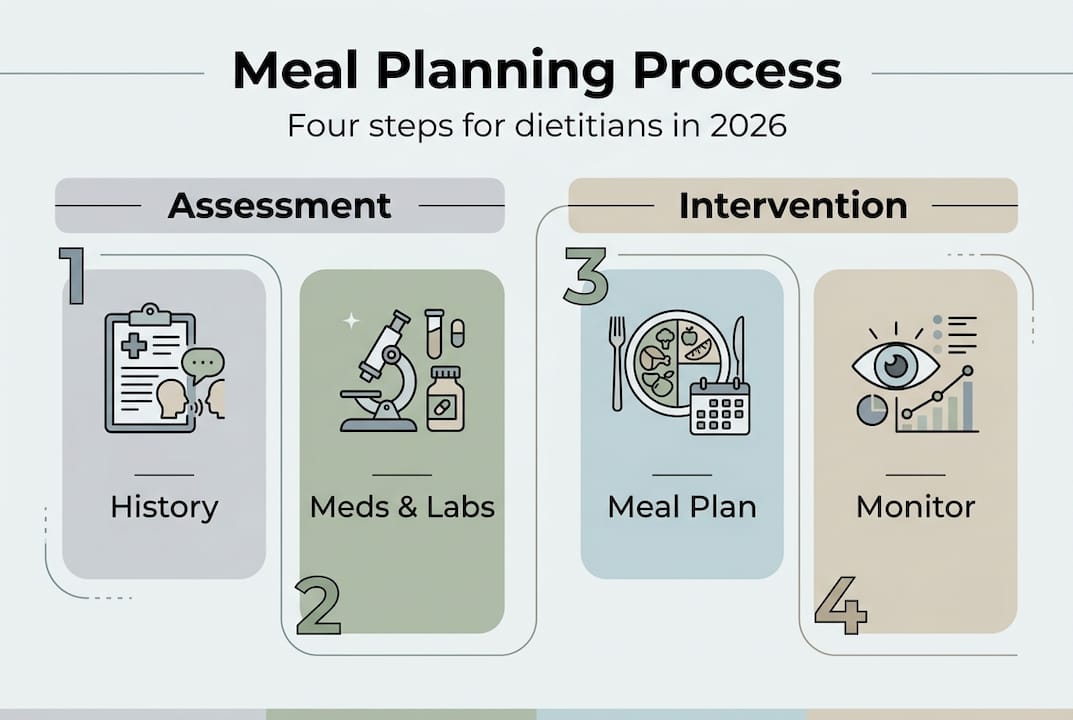
Monitoring and Evaluation closes the loop. You track adherence, measure clinical markers, gather patient feedback, and adjust plans based on results. This isn't a one-time check, it's ongoing optimization. AI-powered meal planning tools can automate much of this tracking, flagging patients who need attention and suggesting evidence-based adjustments.
The NCP's power lies in its systematic nature. Each step builds on the previous one, creating a logical progression from data collection to measurable outcomes. This structure protects you professionally while ensuring patients receive care grounded in their unique circumstances rather than generic templates.
Personalizing meal plans: blending traditional and functional medicine approaches
Conventional medical nutrition therapy provides excellent disease-specific guidelines, but functional medicine adds depth by addressing root causes rather than just managing symptoms. Merging these approaches creates meal plans that work with patients' biochemistry instead of against it.
Functional medicine emphasizes comprehensive root cause analysis using detailed lab work beyond standard panels. You're looking at inflammatory markers, nutrient deficiencies, gut health indicators, and hormone balance. These insights reveal why conventional plans might fail. A patient struggling with a low-fat diet might have gallbladder dysfunction or fat malabsorption, information that completely changes your intervention strategy.

Dietary trigger identification becomes systematic rather than random. Instead of generic elimination diets, you use patient history, symptom patterns, and sometimes food sensitivity testing to pinpoint problematic foods. Common triggers include gluten, dairy, soy, and high-FODMAP foods, but individual responses vary dramatically. Removing the right triggers can resolve symptoms conventional approaches couldn't touch.
Phased transitions matter more than perfect plans. Research shows gradual dietary changes increase adherence by 73% compared to abrupt overhauls. You might start by improving breakfast quality, then address snacking patterns, then optimize dinner composition over several weeks. Each successful phase builds confidence and habits that support the next change.
| Approach Element | Traditional MNT | Functional Medicine Enhancement |
|---|---|---|
| Assessment focus | Disease diagnosis, anthropometrics, basic labs | Root cause analysis, comprehensive biomarkers, timeline mapping |
| Dietary framework | Evidence-based guidelines for conditions | Personalized elimination, nutrient density, anti-inflammatory focus |
| Implementation | Education and meal plans at visit | Phased transitions with symptom tracking between visits |
| Monitoring | Weight, labs, adherence at follow-ups | Continuous symptom logs, functional markers, quality of life metrics |
Pro Tip: Start functional assessments with a detailed timeline connecting life events, symptom onset, and dietary patterns. Patients often reveal crucial connections they didn't think were relevant, like digestive issues starting after antibiotic use or energy crashes correlating with specific foods.
Nutrient density becomes your planning compass. Rather than just hitting macronutrient targets, you prioritize foods that deliver maximum vitamins, minerals, and phytonutrients per calorie. This approach naturally emphasizes vegetables, quality proteins, healthy fats, and strategic carbohydrates while minimizing processed foods. Patients feel better faster because you're addressing deficiencies while managing their primary condition.
Time-restricted eating offers another personalization tool. Some patients benefit from compressed eating windows that support metabolic health and reduce inflammation. You might implement 12-hour overnight fasts initially, then adjust based on response. This isn't appropriate for everyone, but for insulin-resistant or inflammatory conditions, it can accelerate results.
Integrating these approaches requires clinical judgment. You're balancing evidence-based medical nutrition therapy with patient-centered functional medicine principles that address individual biochemistry. Neither approach alone captures the full picture. Together, they create meal plans that manage disease while optimizing function, leading to better adherence and outcomes than either framework achieves independently. AI tools designed for functional medicine can help synthesize these complex data points into coherent, actionable plans.
Executing the meal planning process efficiently while maintaining flexibility
Efficient execution separates meal plans that patients follow from beautiful documents that gather dust. You need systematic steps that create clarity without rigidity, allowing adaptation as real life interferes with perfect intentions.
Your development process follows a logical sequence. First, synthesize assessment data into clear nutrition priorities. What are the top three things this patient needs to change? Second, establish specific, measurable goals with the patient, not for them. Third, design macronutrient distribution appropriate for their condition and preferences. Fourth, build in habit formation strategies that make adherence automatic rather than effortful. Fifth, anticipate obstacles and create troubleshooting protocols before problems arise.
Flexibility proves essential in real-world implementation. Busy days happen. Leftovers accumulate. Family preferences conflict with patient needs. Comorbidities create competing dietary requirements. Your meal plans must accommodate these realities or patients abandon them within days. Build in swap options, simplified backup meals, and clear guidance on when perfection matters versus when good enough is actually good enough.
- Weekly planning sessions: Schedule 30 to 60 minutes for patients to review their upcoming week, identify high-risk situations, and prep accordingly. This prevents decision fatigue when they're tired and hungry.
- Modular meal components: Create mix-and-match protein, vegetable, and carbohydrate options rather than rigid recipes. Patients can assemble meals that fit their schedule and preferences while hitting nutritional targets.
- Scaling strategies: Teach patients how to adjust portions and ingredients based on who's eating and what's available, maintaining nutritional balance without following recipes exactly.
- Recovery protocols: When patients deviate from plans, which they will, provide clear guidance for getting back on track without guilt or compensation behaviors that create new problems.
Pro Tip: Create a simple one-page decision tree for common scenarios like eating out, traveling, or feeling too tired to cook. This reduces the cognitive load of maintaining dietary changes during stressful situations.
Comparing rigid versus flexible approaches reveals stark differences in patient outcomes:
| Planning Approach | Adherence Rate | Patient Satisfaction | Long-term Sustainability | Clinical Marker Improvement |
|---|---|---|---|---|
| Rigid meal plans | 35 to 45% | Low to moderate | Poor | Inconsistent |
| Flexible frameworks | 65 to 80% | High | Good | Consistent |
Special populations require adapted approaches. Eating disorder recovery demands careful collaboration with mental health professionals, avoiding rigid rules that trigger disordered patterns. Inpatient settings need plans that work within institutional food service constraints. Pediatric cases must balance child preferences with parental implementation capacity. AI tools can help customize plans for these complex scenarios, generating options that meet clinical requirements while respecting practical limitations.
Regular plan updates maintain relevance. Schedule touchpoints every two to four weeks initially, then extend as patients stabilize. Each session reviews what worked, what didn't, and why. You're teaching patients to become their own meal planning experts over time, gradually reducing their dependence on your detailed guidance. This approach improves both adherence and patient satisfaction compared to static plans that ignore evolving needs.
Efficiency comes from systems, not shortcuts. Develop templates for common conditions, but customize them during patient interactions. Use evidence-based checklists that ensure you cover essential elements without reinventing the wheel for each patient. Document clearly so you can quickly review and adjust at follow-ups. The goal is spending your limited time on clinical thinking and patient interaction, not administrative tasks that technology can handle.
Verifying results: monitoring, evaluation, and continuous improvement of meal plans
Meal plan success depends on systematic verification. Without structured monitoring, you're guessing whether interventions work or wasting time on ineffective approaches. Effective evaluation combines objective data with subjective patient experience to create a complete picture of progress.
Start with clear adherence metrics. How often is the patient following the plan? Which components are easy versus difficult? Where do deviations occur and why? You need this granular information to distinguish between plans that don't work and plans patients can't execute. The solutions differ dramatically.
Regular monitoring improves adherence rates up to 80% compared to infrequent check-ins. Frequent feedback loops, whether through apps, brief calls, or messaging, keep patients accountable and allow rapid course corrections. When patients know they'll report progress soon, they're more likely to stay on track. When problems arise, early detection prevents small issues from becoming major setbacks.
Clinical markers provide objective outcome data. Track relevant labs, anthropometrics, blood pressure, or other condition-specific indicators at appropriate intervals. Studies show metabolic improvements typically emerge within 3 to 6 months of consistent dietary changes. If markers aren't improving on that timeline, your plan needs adjustment regardless of reported adherence.
- Establish baseline measurements for all relevant clinical and functional markers before implementing meal plans.
- Schedule systematic follow-up testing at intervals appropriate for the condition and intervention intensity.
- Compare results against established targets and patient-specific goals set during the intervention phase.
- Analyze patterns between adherence data, symptom reports, and objective markers to identify what's driving outcomes.
- Adjust plans based on findings, intensifying what works and modifying what doesn't, then monitor the impact of changes.
Patient-reported outcomes matter as much as lab values. Energy levels, sleep quality, digestive symptoms, mood, and overall quality of life tell you whether the plan is sustainable long-term. Research confirms that dietary interventions improving both clinical markers and quality of life achieve better adherence than those focusing solely on disease management.
"Meal planning reduces decision fatigue and food waste while significantly enhancing dietary adherence across diverse patient populations. The systematic approach of planning, preparing, and monitoring creates sustainable behavior change that reactive meal-by-meal decisions cannot achieve."
Technology streamlines the monitoring burden. AI-powered nutrition platforms can track patient logs, flag concerning patterns, and suggest evidence-based adjustments based on accumulated data. This allows you to manage larger caseloads without sacrificing care quality, as the system handles routine monitoring while alerting you to patients needing direct attention.
Continuous improvement requires honest evaluation of your own practice patterns. Which types of patients do best with your approaches? Where do you see consistent struggles? Are there emerging research findings you should incorporate? Professional development in meal planning isn't optional, it's essential for maintaining clinical effectiveness as evidence evolves.
The verification phase completes the cycle, feeding insights back into your assessment and intervention approaches. Each patient interaction teaches you something about what works in real-world conditions. Capturing and applying these lessons systematically elevates your entire practice, transforming you from someone who creates meal plans into someone who engineers sustainable dietary behavior change.
Enhance your meal planning with Meelio AI assistant
Mastering the meal planning process requires balancing clinical expertise with practical efficiency. You've learned the frameworks, but executing them consistently while managing a full caseload demands smart tools that amplify your skills rather than replace them.
Meelio's AI-powered meal planning platform integrates directly with your clinical workflow, automating repetitive tasks while maintaining the personalization your patients need. Generate customized meal plans in minutes instead of hours, incorporating patient preferences, lab results, and condition-specific protocols seamlessly. Our system learns from your practice patterns, suggesting adjustments based on what works for your patient population. Nutritionists using Meelio report saving over four hours daily on meal planning and documentation tasks, time they redirect toward patient interaction and clinical thinking. The platform supports complex functional medicine protocols while integrating with EHR systems you already use. Discover how Meelio transforms integrative clinical practice by combining AI efficiency with practitioner expertise, helping you deliver better patient outcomes without burning out on administrative tasks.
FAQ
What key assessments guide the meal planning process for dietitians?
Comprehensive assessment includes medical history, current medications, lifestyle patterns, detailed dietary intake analysis, relevant biochemical markers, and functional health indicators. Nutrition diagnosis then identifies specific nutrition-related problems using standardized terminology, creating clear targets for meal plan interventions. This systematic approach ensures plans address root causes rather than just symptoms.
How can meal plans be adjusted for patients with multiple comorbidities?
Use flexible frameworks that prioritize the most critical conditions first, then layer additional considerations as patients stabilize. Phased implementation prevents overwhelming patients with too many simultaneous changes. AI tools can help identify compatible interventions across multiple conditions, while coordination with other healthcare providers ensures dietary recommendations align with overall treatment plans.
What role does patient adherence play in successful meal planning?
Adherence directly determines clinical outcomes, as even perfect plans fail if patients can't follow them. Higher adherence correlates with better metabolic markers, symptom improvement, and long-term health outcomes. Gradual transitions and patient-centered flexibility significantly improve adherence rates compared to rigid, one-size-fits-all approaches. Building plans around patient preferences and practical constraints creates sustainable behavior change.
How can AI support dietitians in the meal planning process?
AI reduces time spent on repetitive tasks like generating meal options, calculating macronutrients, and creating shopping lists, freeing clinicians for higher-level clinical thinking. Advanced AI platforms enable rapid customization based on patient data, preferences, and clinical protocols, improving both efficiency and personalization. Automated monitoring flags patients needing attention and suggests evidence-based adjustments, allowing dietitians to manage larger caseloads without sacrificing care quality.





