Patient-centered care for functional medicine: 2026 guide
Discover patient-centered care strategies for functional medicine clinicians. Learn frameworks, evidence-backed tactics, and AI tools to boost engagement and outcomes in 2026.

Patient-centered care goes far beyond empathy or politeness. In functional medicine, it's a rigorous integration of each patient's biochemical individuality, values, and health story into every clinical decision. This approach transforms care plans from generic protocols into personalized roadmaps that respect root causes and honor patient autonomy. You'll discover actionable frameworks, evidence-backed strategies, and technology tools to implement patient-centered care effectively in your integrative practice.
Table of Contents
- Introduction To Patient-Centered Care In Functional Medicine
- Role Of Registered Dietitians And Functional Medicine Clinicians
- Impact Of Patient-Centered Care On Engagement And Outcomes
- Common Misconceptions About Patient-Centered Care
- Comparison Of Functional Medicine Patient-Centered Care With Conventional Models
- Implementing Patient-Centered Care: Practical Strategies And Tools
- Toward Improved Patient Engagement And Outcomes
- Enhance Your Practice With AI-Powered Patient-Centered Tools
- Frequently Asked Questions
Key takeaways
| Point | Details |
|---|---|
| Patient-centered care defined | Integrates patient preferences, values, and biology into personalized functional medicine care plans. |
| RDN and clinician roles | Updated 2025 standards require competence in delivering ethical, person-centered integrative nutrition care. |
| Proven outcomes | Patient-centered RDN care increases satisfaction and adherence by 20-30% with measurable health improvements. |
| Functional vs. conventional | Functional medicine prioritizes root causes and shared decision-making over symptom-focused protocols. |
| Implementation strategies | Practical workflows and AI tools automate personalized care planning, saving clinicians 4+ hours daily. |
Introduction to patient-centered care in functional medicine
Patient-centered care integrates patients' preferences, values, and beliefs into every aspect of health decision-making. For functional medicine clinicians, this means honoring each patient's unique biochemical makeup, environmental exposures, and health narratives to address root causes rather than surface symptoms. Unlike conventional models that apply standardized protocols, functional medicine demands a systems biology perspective where lifestyle, nutrition, genetics, and patient goals shape personalized interventions.
This approach is indispensable because chronic disease requires deep understanding of individual context. You can't reverse metabolic dysfunction or autoimmune conditions with cookie-cutter advice. Patient-centered care in functional medicine builds on core principles that make personalized healing possible:
- Shared decision-making where patients actively participate in selecting interventions
- Continuous engagement through regular follow-up and care plan adjustments
- Respect for patient autonomy and informed consent at every step
- Integration of patient preferences into nutrition, supplement, and lifestyle recommendations
- Focus on root-cause analysis using patient history, labs, and environmental factors
These principles create a foundation for sustainable behavior change. When patients feel heard and see their values reflected in care plans, adherence skyrockets and outcomes improve dramatically.
Role of registered dietitians and functional medicine clinicians
Registered Dietitian Nutritionists practicing integrative and functional medicine deliver nutrition and lifestyle plans that honor biochemical individuality and personal preferences, strengthening patient-centered care and dietary behaviors. RDNs translate complex functional medicine protocols into actionable meal plans, supplement regimens, and lifestyle modifications tailored to each patient's biology and goals. This role extends far beyond basic nutrition counseling.
The 2025 Revised Scope and Standards of Practice emphasize competence in delivering safe, ethical, person-centered care with ongoing self-evaluation and continuing education. These updated standards require RDNs to:
- Demonstrate expertise in integrative and functional nutrition principles
- Maintain ethical practice through informed consent and transparent communication
- Personalize interventions based on patient genetics, microbiome, and metabolic status
- Collaborate with multidisciplinary teams including physicians, health coaches, and therapists
- Pursue continuing education to stay current with evolving functional medicine research
Pro Tip: Regularly assess your practice against the 2025 standards to ensure you're meeting competence benchmarks and delivering the highest quality patient-centered care.
Functional medicine clinicians and RDNs work best when they integrate complementary expertise. RDNs bring deep nutrition science while clinicians manage medical oversight and complex protocols. Using an AI assistant for nutritionists can streamline personalized plan creation, freeing time for deeper patient interaction and collaborative care.

Impact of patient-centered care on engagement and outcomes
Patients receiving patient-centered care from RDNs report higher satisfaction and adherence, with improvements by 20-30% in nutrition-related health behaviors. This data confirms what clinicians observe daily: when patients co-create their care plans and feel genuinely heard, they stick with recommendations and see measurable progress. Patient-centered approaches empower individuals through shared decision-making, building trust that transforms therapeutic relationships.
The positive impacts extend across multiple outcome domains:
| Outcome Measure | Improvement |
|---|---|
| Patient satisfaction | 25-30% increase |
| Treatment adherence | 20-25% increase |
| Nutrition behavior change | 20-30% improvement |
| Therapeutic relationship quality | Significant strengthening |
| Clinical biomarker progress | Faster improvement rates |
These gains translate into real clinical wins. Patients adopting personalized nutrition plans experience faster normalization of inflammatory markers, improved insulin sensitivity, and better energy levels. Behavioral changes linked to patient-centered nutrition include:
- Sustained dietary modifications aligned with personal food preferences
- Increased willingness to try new foods and cooking methods
- Better supplement compliance when patients understand the "why" behind recommendations
- More proactive communication about challenges and side effects
- Higher retention in longitudinal care programs
Understanding integrative health outcomes helps you measure these improvements systematically. When patients see their lab values improve and symptoms resolve, motivation compounds and long-term adherence becomes the norm.
Common misconceptions about patient-centered care
Many clinicians mistakenly believe patient-centered care merely means being polite or empathetic. In reality, it requires active integration of patients' unique biology, preferences, and values into clinical decision-making, supported by ongoing dialogue and shared decision-making. This misconception leads to superficial application where clinicians nod sympathetically but still impose standardized protocols.
Patient-centered care in functional medicine demands operational frameworks, not vague concepts. You need structured intake processes, collaborative goal-setting sessions, and systems for tracking patient preferences across visits. Without these, "patient-centered" becomes empty rhetoric.
Frequent misconceptions include:
- Believing patient-centered care means giving patients whatever they want, ignoring clinical evidence
- Thinking empathy alone substitutes for integrating patient values into treatment plans
- Assuming patient-centered approaches take too much time without workflow optimization
- Confusing patient-centered care with patient satisfaction surveys or politeness training
- Overlooking the need to honor biochemical individuality, not just emotional preferences
Functional medicine's patient-centered model is distinct because it integrates root-cause analysis with patient narrative. You're not just asking what patients want; you're discovering their unique physiological drivers and co-creating interventions that align with their lives. This depth separates true patient-centered care from conventional care's surface-level attempts.
Comparison of functional medicine patient-centered care with conventional models
Functional medicine emphasizes root causes, patient narrative, and personalized plans built on systems biology. Conventional care often focuses on symptom suppression using standardized protocols that ignore individual context. This fundamental difference shapes every aspect of patient interaction.
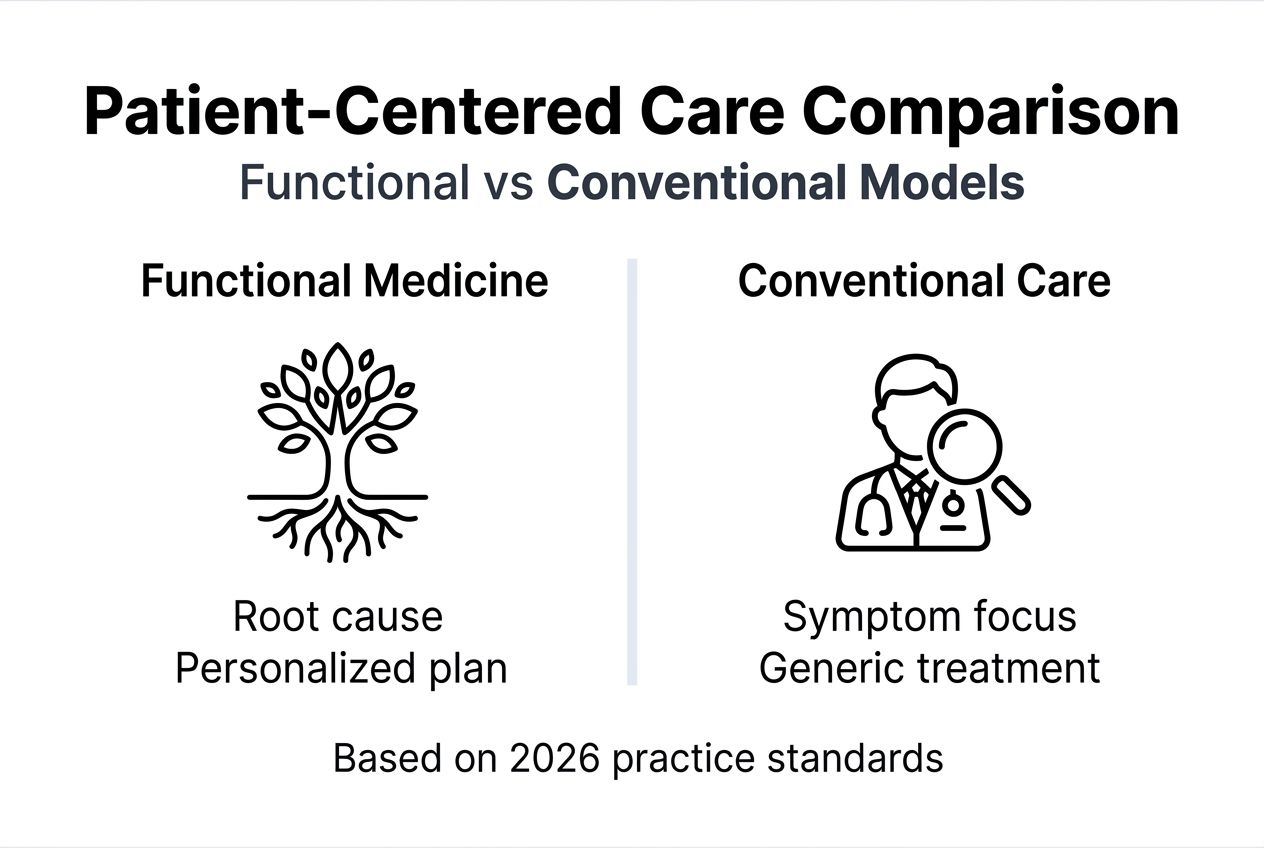
| Aspect | Functional Medicine Patient-Centered Care | Conventional Care |
|---|---|---|
| Focus | Root-cause analysis and systems biology | Symptom management |
| Treatment approach | Personalized plans based on biochemical individuality | Standardized protocols |
| Patient role | Active partner in shared decision-making | Passive recipient of prescriptions |
| Timeline | Long-term healing and prevention | Short-term symptom relief |
| Data integration | Genetics, lifestyle, environment, labs, patient story | Labs and symptoms only |
In functional medicine, you spend time understanding genetic predispositions, environmental exposures, gut health, and stress patterns. This integrated context informs every recommendation. Conventional models rarely account for these layers, leading to interventions that may relieve symptoms temporarily but fail to address underlying dysfunction.
Patient engagement transforms when you prioritize root-cause discussions. Instead of telling patients to "eat healthier," you explain how their specific methylation issues require targeted B-vitamin support or how their histamine intolerance drives their migraines. This specificity builds trust and compliance.
Key advantages of functional medicine's patient-centered model:
- Honors each patient's unique metabolic and genetic profile
- Integrates lifestyle factors like sleep, stress, and movement into care plans
- Uses shared decision-making to align interventions with patient values
- Tracks longitudinal data to adjust plans as patient needs evolve
- Focuses on sustainable behavior change, not quick fixes
Pro Tip: Lead every patient visit with root-cause questions rather than symptom checklists to build trust and position yourself as a partner in healing, not just a symptom manager.
Implementing patient-centered care: practical strategies and tools
Effective patient-centered care requires structured workflows and technology support to scale personalized interventions without burnout. Start with a stepwise implementation framework:
- Conduct comprehensive patient assessments using detailed intake forms that capture health history, values, and goals
- Facilitate shared decision-making sessions where you present options and co-create priorities
- Generate personalized care plans integrating nutrition, supplements, lifestyle, and labs
- Enable tech-supported follow-up with automated tracking and patient communication tools
- Review and adjust plans based on longitudinal lab data and patient feedback
AI tools like Meelio automate care plan generation, saving clinicians 4+ hours per day while maintaining personalization. These platforms analyze patient data, apply protocol-specific intelligence for frameworks like Bredesen or Wahls, and generate individualized nutrition recommendations instantly. Technology's role extends to:
- Longitudinal lab tracking that flags trends and suggests interventions
- Automated meal planning aligned with patient dietary preferences and restrictions
- Integration with EHRs like Practice Better and Cerbo for seamless workflows
- Protocol-specific clinical intelligence that goes beyond generic AI scribes
Practical strategies to enhance patient-centered care:
- Use patient intake data to personalize every interaction from the first visit
- Schedule longer initial consultations to build rapport and gather comprehensive histories
- Implement patient management workflows that prioritize continuous engagement
- Leverage AI care plans to reduce documentation burden and increase face time
- Deploy AI medical scribe technology to capture visit details without distraction
Pro Tip: Leveraging AI reduces burnout by eliminating repetitive tasks, freeing you to focus on high-value patient interactions that build trust and drive adherence.
Meal planning boosts adherence by translating abstract dietary advice into concrete weekly menus. When patients receive personalized grocery lists and recipes, compliance soars. AI assistants for nutritionists generate these resources in minutes, making personalized meal planning scalable.
Toward improved patient engagement and outcomes
Patient-centered care is the essential foundation for functional medicine success. Without it, even the most sophisticated protocols fail because patients don't adhere or trust the process. By embracing personalized nutrition and care plans that honor each patient's unique biology and values, you create conditions for sustainable healing.
Technology plays a critical role in enabling scalable, efficient patient-centered workflows. AI-powered platforms automate time-consuming tasks like care plan generation and meal planning, allowing you to deliver personalized care without burnout. This combination of human expertise and intelligent automation is the future of integrative medicine.
Commit to continuous learning and technology adoption. The 2025 practice standards and emerging AI tools give you everything needed to deliver world-class patient-centered care. Meal planning AI saves 4+ hours daily, freeing time for deeper patient relationships and better outcomes. Explore Meelio's AI assistant platform to see how technology can transform your practice today.
Enhance your practice with AI-powered patient-centered tools
Ready to operationalize patient-centered care at scale? Meelio's AI assistant is built specifically for integrative and functional medicine clinicians like you. Our platform automates personalized care plan generation, meal planning, and longitudinal lab analysis, saving you 4+ hours daily while improving patient engagement and outcomes.
Unlike generic AI scribes, Meelio delivers protocol-specific clinical intelligence for complex frameworks like Bredesen, Shoemaker, and Wahls. Integrate seamlessly with your EHR and start delivering truly personalized care without the administrative burden. Explore AI care plans and AI meal planning solutions to see how Meelio transforms patient-centered workflows.
Frequently asked questions
What is the difference between patient-centered care and functional medicine?
Patient-centered care is a care delivery philosophy that integrates patient preferences and values into decision-making. Functional medicine is a clinical framework focusing on root-cause analysis and systems biology. When combined, patient-centered functional medicine delivers personalized, root-cause interventions that honor each patient's unique biology and goals.
How can registered dietitians best support patient-centered care?
RDNs support patient-centered care by personalizing nutrition plans based on biochemical individuality, engaging patients in shared decision-making, and maintaining continuous communication. Using the 2025 practice standards, RDNs ensure ethical, competent care while collaborating with multidisciplinary teams to address complex functional medicine cases.
What are practical first steps to implement patient-centered care?
Start with comprehensive patient intake forms that capture health history, values, and goals. Schedule longer initial consultations to build rapport and co-create priorities. Implement technology tools for automated care plan generation and follow-up tracking. Review patient feedback regularly to refine your workflows and ensure you're truly integrating patient preferences.
How does technology enhance patient-centered care in practice?
Technology automates time-consuming tasks like care plan documentation, meal planning, and lab tracking, freeing clinicians to focus on patient interaction. AI platforms analyze patient data and generate personalized recommendations instantly, making individualized care scalable. EHR integrations ensure seamless workflows and comprehensive patient records.
What outcomes can clinicians expect from patient-centered approaches?
Clinicians implementing patient-centered care see 20-30% improvements in patient satisfaction and adherence. Clinical biomarkers improve faster, therapeutic relationships strengthen, and patients demonstrate sustained behavior change. Long-term retention increases as patients feel genuinely heard and see measurable progress in their health.
How does patient-centered care reduce clinician burnout?
By leveraging AI tools to automate repetitive documentation and care plan generation, clinicians reclaim 4+ hours daily for meaningful patient interactions. This shift from administrative burden to high-value care increases job satisfaction and reduces burnout. Technology enables you to deliver personalized care at scale without working longer hours.





