What is a care plan? A guide for functional medicine
Discover what functional medicine care plans are, how they differ from conventional protocols, and practical steps to create personalized clinical workflows that improve patient outcomes.

Many practitioners mistakenly view care plans as static, one-size-fits-all protocols borrowed from conventional medicine. In reality, functional medicine care plans are dynamic, personalized clinical workflows that integrate patient history, lifestyle factors, and targeted nutrition guidance to address root causes of chronic illness. This guide clarifies what functional medicine care plans truly involve, the essential steps to develop them, and how to apply them effectively to improve patient outcomes and streamline your practice.
Table of Contents
- Understanding Care Plans In Functional Medicine
- Steps To Develop And Execute A Functional Medicine Care Plan
- Systems-Based Approach And Nuanced Challenges In Care Planning
- Applying Care Plans Effectively: Practical Tips And Examples
- Enhance Your Care Plans With Meelio AI Tools
- Frequently Asked Questions
Key takeaways
| Point | Details |
|---|---|
| Care plans are personalized protocols | They target root causes of chronic illness rather than merely managing symptoms. |
| Three core implementation steps | Assessment of patient factors, tailored intervention including nutrition, and ongoing monitoring for adaptation. |
| Nutrition and lifestyle are central | Dietary modifications, stress management, and behavioral changes form the backbone of effective care plans. |
| Systems-based thinking is essential | Functional medicine addresses interconnected body systems like the gut-immune axis rather than isolated symptoms. |
| Technology streamlines execution | AI-powered tools reduce administrative burden while maintaining personalized clinical workflows. |
Understanding care plans in functional medicine
Functional medicine protocols are structured care plans designed to address underlying factors contributing to chronic conditions. Unlike conventional treatment protocols that focus on symptom suppression, these plans identify and treat root causes through comprehensive patient assessment and individualized interventions. Personalized clinical workflows integrate lifestyle modifications and nutrition guidance to reverse or manage complex health issues at their source.
A typical functional medicine care plan includes several key components working together. Dietary interventions target inflammation, optimize gut health, and balance hormones. Supplementation addresses nutrient deficiencies and supports cellular function. Stress management techniques like meditation or breathwork regulate the hypothalamic-pituitary-adrenal axis. Sleep optimization protocols restore circadian rhythm. Movement prescriptions enhance metabolic health and reduce systemic inflammation.
These elements form an integrated approach rather than isolated interventions. For example, improving gut health through dietary changes often simultaneously reduces inflammation, enhances nutrient absorption, and stabilizes mood. This interconnected strategy reflects the core philosophy of functional medicine where body systems influence each other dynamically.
Pro Tip: Invest time in thorough initial assessment. The quality of your care plan depends entirely on understanding the patient's unique biochemistry, environmental exposures, genetic predispositions, and lifestyle patterns. Rushing this foundation compromises everything that follows.
The shift toward patient-centered care in functional medicine requires practitioners to view care plans as living documents. They evolve as patients progress, new information emerges from testing, and individual responses to interventions become clear. This adaptive approach contrasts sharply with static protocols common in conventional settings.
Steps to develop and execute a functional medicine care plan
Three key steps define functional medicine protocols: assessment, intervention, and monitoring. Each phase requires careful attention to detail and continuous refinement based on patient response.
-
Comprehensive assessment phase: Gather detailed patient history including childhood health events, environmental exposures, stress timeline, and family health patterns. Order baseline labs covering thyroid function, inflammatory markers, nutrient levels, and metabolic panels. Evaluate lifestyle factors including diet quality, sleep patterns, physical activity, and stress management practices. Consider advanced testing like organic acids, microbiome analysis, or food sensitivity panels when indicated.
-
Individualized intervention design: Create phased protocols starting with foundational interventions like dietary changes and basic supplementation. Layer additional strategies as patients demonstrate readiness and response. Prioritize interventions based on patient preferences, financial constraints, and likelihood of adherence. Integrate nutrition as the primary therapeutic tool, using supplements to support rather than replace dietary improvements. Address psychological and emotional factors that influence health outcomes.
-
Ongoing monitoring and adaptation: Schedule regular follow-ups to track progress through subjective reports and objective measures. Adjust protocols based on patient response, emerging symptoms, or lab value changes. Educate patients continuously about the rationale behind interventions to improve adherence. Celebrate small wins to maintain motivation during long treatment timelines.
Functional medicine consults require more time with patients compared to conventional visits, creating billing and scheduling challenges. Initial appointments often span 60 to 90 minutes, with follow-ups requiring 30 to 45 minutes. This time investment allows for thorough assessment and patient education but demands careful practice management.
Pro Tip: Develop standardized functional health assessment checklists that capture essential information efficiently. Templates ensure you collect comprehensive data without reinventing the process for each patient, balancing thoroughness with time management.
Systems-based approach and nuanced challenges in care planning
Systems-based thinking considers interconnected body systems and addresses imbalances at the cellular level. The gut-immune axis exemplifies this interconnectedness where intestinal permeability triggers systemic inflammation, autoimmune reactions, and neurological symptoms. Hormone imbalances often trace back to liver detoxification issues, microbiome dysbiosis, or chronic stress. Understanding these relationships prevents practitioners from treating symptoms in isolation.
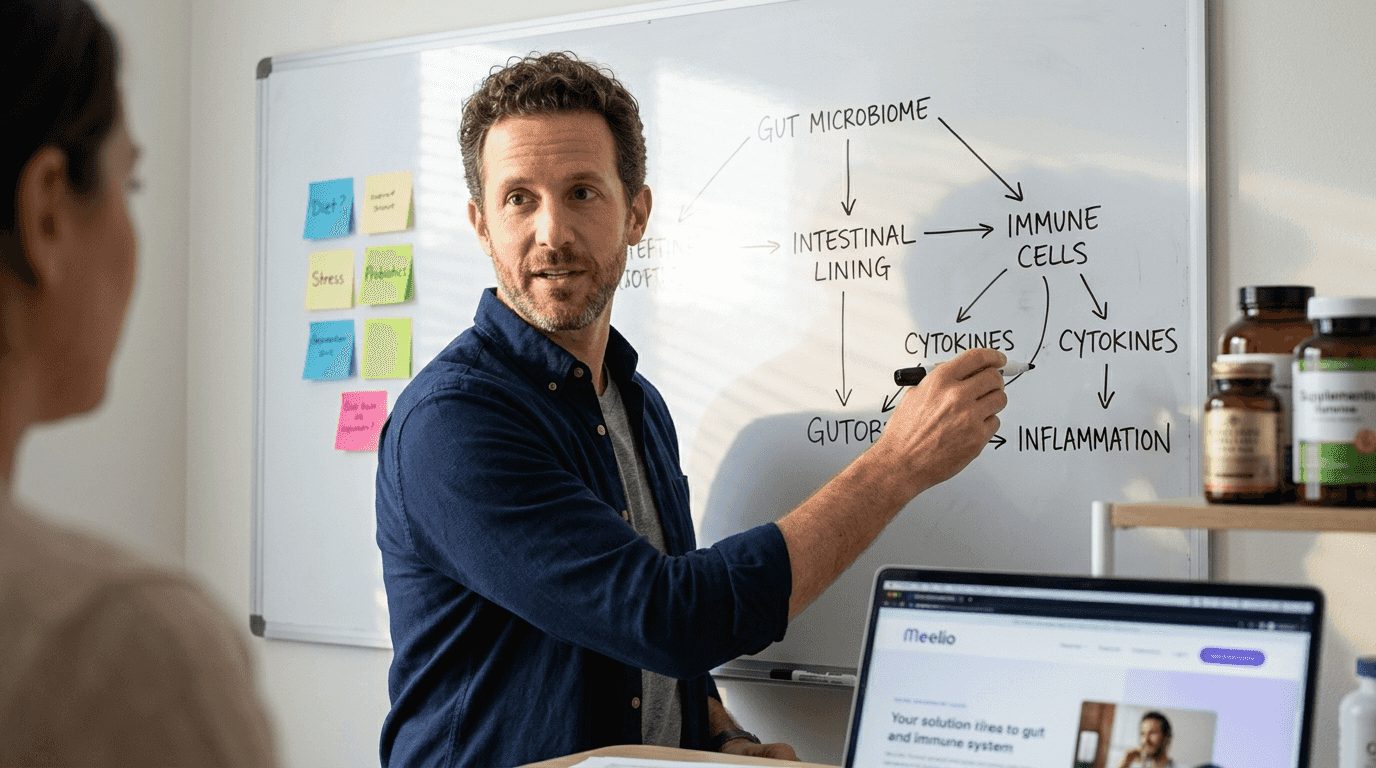
Advanced diagnostics reveal system-level dysfunctions invisible to standard labs. Comprehensive stool analysis identifies pathogenic overgrowth, beneficial bacteria deficiencies, and digestive enzyme insufficiency. Food sensitivity testing uncovers hidden inflammatory triggers. Organic acid testing assesses mitochondrial function, neurotransmitter metabolism, and detoxification capacity. Hormone panels map circadian rhythm disruptions and feedback loop dysregulation.
Complex, multi-systemic illnesses present edge cases where identifying primary drivers proves challenging. Patients with multiple autoimmune conditions, chronic infections, mold exposure, and metabolic dysfunction require layered protocols addressing multiple systems simultaneously. Prioritizing interventions becomes critical when everything appears dysfunctional.
| Challenge | Best Practice |
|---|---|
| Over-reliance on supplements | Prioritize dietary and lifestyle changes as primary interventions, using supplements strategically |
| Ignoring patient readiness | Assess motivation and capacity before prescribing complex protocols |
| Treating lab values instead of patients | Balance objective data with subjective experience and functional capacity |
| Neglecting conventional care integration | Collaborate with conventional providers, especially for acute conditions or medication management |
Common pitfalls include overwhelming patients with too many interventions simultaneously. Starting with 15 supplements, strict elimination diets, and multiple lifestyle changes often leads to poor adherence and patient burnout. Phased approaches build sustainable habits and allow you to identify which interventions drive improvement.
Another mistake involves inadequate patient education. When patients don't understand why they're taking specific supplements or following dietary restrictions, compliance plummets. Invest time explaining mechanisms, expected timelines, and how interventions address their specific imbalances. Use analogies and visual aids to make complex biochemistry accessible.
Leveraging workflow automation in functional medicine helps practitioners manage the complexity inherent in systems-based care plans without sacrificing personalization. Technology handles repetitive tasks while you focus on clinical reasoning and patient relationships.
Applying care plans effectively: practical tips and examples
Integrating lifestyle modifications and nutrition guidance into personalized clinical workflows requires practical strategies that balance evidence-based interventions with individual patient contexts. Start with nutrition as your primary therapeutic modality. An anti-inflammatory diet eliminating processed foods, refined sugars, and common allergens often produces dramatic improvements in energy, pain levels, and mental clarity within weeks.
Phased protocols allow patients to integrate changes gradually. Begin with basic dietary improvements and foundational supplements like vitamin D, magnesium, and omega-3 fatty acids. Once patients demonstrate adherence and initial response, layer in targeted interventions addressing specific imbalances revealed through testing. This approach prevents overwhelm and allows you to attribute improvements to specific interventions.

Documented cases show improvement through phased microbiome restoration and minimal pharmaceutical intervention. Patients with complex, chronic conditions often respond to gut-focused protocols combining antimicrobial herbs, probiotics, prebiotic fibers, and dietary modifications. Addressing the microbiome frequently produces cascading improvements across multiple systems.
| Intervention Type | Timeline to Response | Maintenance Required |
|---|---|---|
| Elimination diet | 2 to 4 weeks | Ongoing food sensitivity management |
| Gut restoration protocol | 3 to 6 months | Periodic microbiome support |
| Adrenal support program | 6 to 12 months | Stress management practices |
| Mitochondrial restoration | 3 to 9 months | Nutrient-dense diet, targeted supplements |
Pro Tip: Use technology to streamline care plan creation and follow-up. AI-powered platforms can generate personalized protocols based on patient data, track adherence patterns, and flag concerning trends between appointments. This frees your cognitive bandwidth for complex clinical reasoning while ensuring consistent, high-quality patient support.
Patient education drives long-term success more than perfect protocols. When patients understand how dietary choices affect inflammation, how stress depletes nutrients, and how sleep impacts hormone balance, they become active participants rather than passive recipients of care. Provide resources, explain mechanisms, and connect interventions to their specific symptoms and goals.
Adapting plans based on individual progress requires regular assessment and open communication. Some patients respond rapidly to interventions while others need months to show measurable improvement. Metabolic flexibility, toxic burden, genetic variants, and stress levels all influence response timelines. Maintain realistic expectations while persistently refining approaches based on results.
Implementing efficient patient management workflows allows practitioners to deliver personalized care at scale. Structured templates, automated reminders, and standardized assessment tools maintain consistency while preserving the individualized attention functional medicine demands. Technology should enhance rather than replace the therapeutic relationship.
The future of functional medicine lies in combining clinical expertise with AI-powered personalized care that analyzes complex patient data, suggests evidence-based interventions, and tracks outcomes across populations. These tools amplify practitioner effectiveness rather than replacing clinical judgment, allowing you to serve more patients without compromising quality.
Enhance your care plans with Meelio AI tools
Developing personalized care plans demands significant time and expertise. Meelio streamlines this process through AI-powered automation designed specifically for integrative and functional health practitioners. Our platform generates customized protocols based on patient-specific data, integrating complex frameworks like Bredesen, Shoemaker, and Wahls without manual protocol lookup.
Automated care plan generation reduces the hours spent creating individualized protocols while maintaining clinical rigor. The system analyzes patient history, lab results, and symptom patterns to suggest evidence-based interventions tailored to each case. AI meal planning features create personalized nutrition guidance aligned with therapeutic goals, saving practitioners hours weekly while enhancing patient adherence through practical, actionable recommendations.
By integrating with EHRs like Practice Better and Cerbo, Meelio fits seamlessly into existing workflows rather than adding another disconnected tool. Practitioners report saving over four hours daily while improving patient outcomes through consistent, protocol-driven care delivery.
Frequently asked questions
What is the typical duration of a functional medicine care plan?
Most functional medicine care plans span three to twelve months for initial protocols, with many patients requiring ongoing maintenance. Acute conditions may resolve in weeks, while reversing chronic illness often demands six months or longer. The timeline depends on condition complexity, patient adherence, and individual healing capacity.
How do functional medicine care plans differ from conventional treatment plans?
Functional medicine care plans target root causes through nutrition, lifestyle, and targeted supplementation rather than primarily managing symptoms with medications. They address multiple body systems simultaneously, recognize biochemical individuality, and evolve based on patient response. Conventional plans typically follow standardized protocols for specific diagnoses.
Are functional medicine care plans covered by insurance?
Insurance coverage for functional medicine remains limited in 2026. Some plans cover initial consultations or specific lab tests, but many interventions like advanced testing, supplements, and extended visit times are out-of-pocket expenses. Practitioners often operate cash-based or hybrid models, and patients should verify coverage before beginning care.
What role does nutrition play in functional medicine care plans?
Nutrition serves as the primary therapeutic intervention in most functional medicine care plans. Dietary changes reduce inflammation, restore gut health, balance hormones, and provide raw materials for cellular function. Food is medicine in functional practice, with supplements supporting rather than replacing nutritional interventions. Personalized nutrition guidance addresses individual sensitivities and metabolic needs.
How often should care plans be updated or modified?
Initial care plans typically require modification every four to eight weeks based on patient response and follow-up testing. As patients progress, adjustment frequency may decrease to every three to six months. Significant life changes, new symptoms, or plateau in progress warrant immediate plan revision regardless of scheduled timeline.





